Crossmatching is a critical process in transfusion laboratories – it ensures that patients receive safe and compatible blood transfusions. Mistakes can have severe, even fatal, consequences. But training scientists to perform this vital test is only getting more difficult.
In a busy NHS, staff shortages, high workloads, and lack of lab space all make it hard to support the kind of 1-on-1 training typically needed to learn how to perform the crossmatch test safely and independently. With experienced staff leaving the profession, even trainers themselves are left with knowledge gaps that are then passed on to trainees.
To try and address these issues, Make Real and NHS Blood and Transplant (NHSBT) developed the Crossmatching VR app. Our goal was to create training that would be as effective as live training sessions – while removing the physical barriers, limitations, risks and expenses, and freeing up time for biomedical scientists (BMSs) to carry out higher-value tasks.
This has been the subject of an extensive and detailed academic study, which has already shown:
Crossmatching VR has been recognised with a Gold Award for Best Use of Simulations at 2025’s Learning Technologies Awards, and the app is being used with all NHSBT’s new starters in their specialised reference service that provide a referral service for complex transfusion cases from 250+ hospitals in England.
Mistakes in the crossmatching procedure can be fatal. In 2024, 17.2% of transfusion errors reported in the UK originated in laboratories, with three leading to death and four leading to major morbidity.
It is exactly this kind of procedural, high-stakes, judgement-heavy skill that VR excels at. We had worked with NHSBT on previous VR experiences, focusing on specific lab processes like aseptic techniques. We’d also created a proof-of-concept experience for blood grouping – so, we knew it was a valid use case.
We knew that with a successful VR deployment, learners would no longer require access to live labs, real patient samples, or physical trainers. It would address the practical barriers and provide a real alternative to face-to-face training.

A student trying the crossmatching VR simulation.
When the Make Real team began building the app, we worked closely alongside NHSBT to match the experience to the learning outcomes. Learners needed to:
There are four key elements to get right in the lab.
The aim was authentic recreation of each element and step in the crossmatching process. Our learning designers actually visited a transfusion lab to practise crossmatching themselves – helping them to understand not just what happens, but how it feels to carry out the process. This way, we could best decide which steps should be fully interactive or could be shown as a simple animation. Interactions like using a pipette were recreated to be as lifelike as possible, being a key step for this process and many other lab processes.

Principal Learning Designer Tim trying out the crossmatching process.
We built three scenarios, each with patients who have different needs for their blood transfusion. These drill into key areas of error, such as getting patient details and specific requirements related to their conditions right, and how these determine the correct red cell unit.
At the end, the red cell units are second-checked by a colleague, replicating what would happen in real life. If an error was made, the colleague explains what went wrong. The patient also explains what impact the error would have on them.
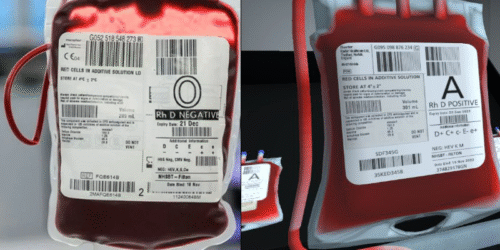
A real red cell unit compared with the simulated one.
As one learner commented:
“At the end of each case, once the final decision had been made the patient outcome was shown. It also lets you see the outcome if it was incorrect. When I made the wrong choice, it was explained where I went wrong. This helped me to understand the impact on the patient of even making one small incorrect choice.”
We designed the VR carefully to make it a comfortable experience, no matter the user’s familiarity with it: single-hand controls, short 15-minute modules, minimal movement required, voiceover and symbol prompts, and fade-to-black transitions to reduce nausea in first-time users.

The Crossmatching app has been the subject of a doctorate research project into the use of VR for transfusion training – with results showing clear learning benefits.
In an initial pilot study, biomedical and healthcare science undergraduate students with no experience in transfusion labs completed the VR training.
All participants:
Following this, a larger scale study was conducted, involving 103 BMS and trainee BMS participants from 43 hospitals and blood centres in England and Wales. These participants were split into an experimental VR group and a control group. And the study showed…
In knowledge assessments, VR is:
When it comes to practical skills…
What does that mean?
It means that VR is a viable alternative to face-to-face training, producing similar if not better results. And VR can actually enable training to happen, without the pressures of time and resource shortages.
81% of the VR participants said they’d recommend the training to others, reporting that the simulation was “easy to follow,” “low-pressure,” and “low-stress”, in contrast to the high-pressure, resource-constrained nature of real transfusion labs.
On top of the benefits for learners, VR is an excellent tool for trainers themselves.
In the control group, half reported negatively about managing to deliver training alongside their usual duties. In the VR group, only 5% reported a negative impact.
Traditional crossmatching training requires costly and time-intensive inputs:
The VR simulation overcomes these constraints by offering scalable, on-demand training with no use of physical consumables or lab time.
And in terms of biomedical scientists’ time, VR could be a crucial tool in freeing them up for vital clinical duties. These BMSs are typically Band 7 NHS employees on higher salaries.
In Red Cell Immunohaematology (RCI) labs, setting up standard face-to-face lab training takes around seven hours:
In face-to-face training in an RCI lab, the training takes 3.5 hours and requires a ratio of one trainer to two learners.
And post-training requires another seven hours:
So, a single in-lab course needs 31.5 hours of a Band 7 biomedical scientist.
Contrast that with the VR training, which requires around two hours of prep, a ratio of one trainer to 10 learners, and six hours of post-training admin. That’s only 11.5 hours – a significant saving of 20 hours which can be spent on other clinical tasks, such as testing real patient samples.

We’re incredibly proud at Make Real to have been involved with this project from the positive learner and trainer feedback…
“This training has emphasised the need for every step to be carried out correctly and why it is important, an error at any step of the way can lead to delayed blood or patient harm.”
“I think this is a great method to implement in our training. Everyone seems excited about this VR training method. The feedback from the participant was very positive.”
…to helping show how VR can support the NHS’s training needs.
If you’d like to read the research yourself, you can find Laura Eastwood’s doctoral thesis here: https://e-space.mmu.ac.uk/view/creators/Eastwood=3ALaura=3A=3A.html
We’re always happy to talk to you about how immersive technologies can engage your employees and customers. If you have a learning objective in mind, or simply want to know more about emerging technologies like VR, AR, or AI, send us a message and we’ll get back to you as soon as we can.